Latest News
Top Stories
- Health & Fitness
- LifeStyle
- Supplements
- Weight Loss
- June 7, 2024
What Should All Men Know About Yeast Infections?
- June 7, 2024
Entertainment or health-which one is necessary
- June 7, 2024
Benefits of Root and Vegetables for the good Health
- June 7, 2024
Best Natural Juice for good Health and Fitness
- June 7, 2024
Coffee and your Health: Benefits and Drawbacks
Diet
- November 18, 2024
Physical Therapy for Abdominal Adhesions: A
- July 7, 2025
Achnical: Supplements to Help with Achalasia
- November 21, 2024
Atrial Fibrillation Cured Naturally: The Ultimate
Health & Fitness
- June 8, 2024
How to Cure Fungal Infection on Skin
- June 8, 2024
Best Supplement & Remedy For Men Health
- June 8, 2024
How Regular Exercise Can Enhance Your Everyday
- June 8, 2024
The Link Between Herbal Diet And Chronic
Bronchiectasis
- adminblog
- November 25, 2024
New Treatments for Bronchiectasis: Hope for a Better Life
Bronchiectasis is a chronic lung condition that can significantly impact
- adminblog
- November 25, 2024
Effective and Natural Bronchiectasis Therapies for Better Breathing
Bronchiectasis is a chronic condition characterized by damaged airways that
- adminblog
- November 25, 2024
Best Sleeping Position for Bronchiectasis: Improve Your Breathing and Comfort
Bronchiectasis, a chronic condition that involves damage to the airways,
Bullous Pemphigoid
- adminblog
- November 26, 2024
Foods to Avoid with Bullous Pemphigoid: What to Cut Out Today

- adminblog
- November 26, 2024
Bullous Pemphigoid vs Pemphigus Vulgaris: Treatment Options You Need to Know
Autoimmune blistering diseases like Bullous Pemphigoid and Pemphigus Vulgaris are
- adminblog
- March 28, 2024
Treating Bullous Pemphigoid Naturally: The Top Supplements to Try
Bullous Pemphigoid is a chronic autoimmune skin disease that causes
- adminblog
- March 21, 2024
Top 5 Natural Treatments for Bullous Pemphigoid
Introduction Bullous pemphigoid (BP) is a skin condition that causes
Burning Mouth Syndrome
- adminblog
- November 27, 2024
Saline Spray Burning Mouth Roof: Simple Remedies for Burning Mouth
Saline Spray Burning Mouth Roof: Simple Remedies for Burning Mouth
- adminblog
- August 24, 2024
How to Avoid Having a Burning Mouth After Eating Spicy Food
We’ve all experienced it: Believing you can handle the heat
- adminblog
- August 5, 2024
Burning Mouth Syndrome Relief: How to Find Comfort and Calm Fast
Burning Mouth Syndrome (BMS) is a perplexing and often painful
More News
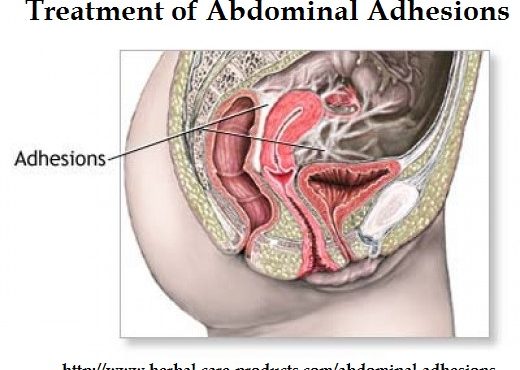
- Abdominal Adhesions
- Achalasia
- Actinic Keratosis
- Alopecia
- adminblog
- March 11, 2024
Natural Treatment for Abdominal Adhesions Reviews 2023
Introduction Abdominal adhesions can be a source of immense discomfort, interfering with daily life and
- adminblog
- March 11, 2024
Diagnosis and Treatment of Abdominal Adhesions
While diagnosing abdominal adhesions, it is important to take a thorough clinical history in order
- adminblog
- March 11, 2024
11 Natural Home Remedies for Abdominal Adhesions
What is Abdominal Adhesion? Intestinal adhesions are bands of scar tissue that form between abdominal
- adminblog
- March 11, 2024
Abdominal Adhesions Natural Herbal Remedies for Pain
Abdominal Adhesions Pain by Herbal Care Products Abdominal Adhesions are strands or of scar tissue
- adminblog
- November 18, 2024
Abdominal Adhesions Diet: What to Eat and Avoid for Relief
Abdominal adhesions are bands of scar tissue that can form in the abdomen, often following
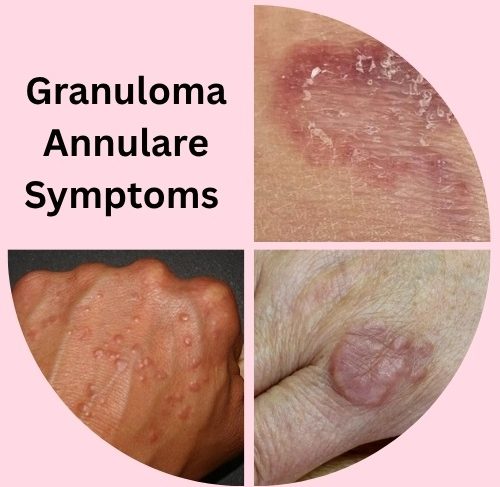
Granuloma Annulare
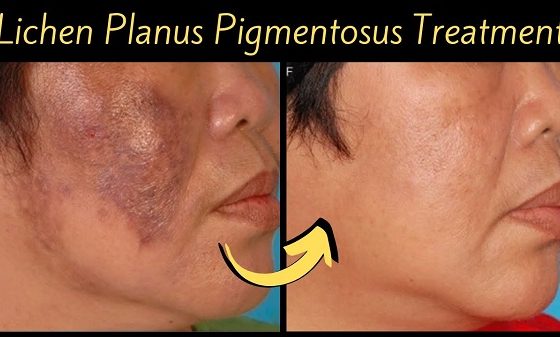
Lichen Planuus
Latest Reviews
- June 26, 2025
How to Treat Arthritis in Hands Effectively:
- June 21, 2025
Arthritis in Hands: Early Symptoms You Shouldn’t
- June 19, 2025
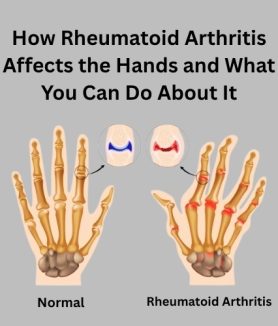
How Rheumatoid Arthritis Affects the Hands and
Featured Categories
- Abdominal Adhesions
- Achalasia
- Actinic Keratosis
- Alopecia
- Atrial Fibrillation
- Benign Essential Tremor
- Blepharitis
- Bronchiectasis
- Bullous Pemphigoid
- Burning Mouth Syndrome
- Cellulitis
- Corona
- Costochondritis
- Delayed Ejaculation
- Diet
- Epididymitis
- Eye Bags
- Flatulence
- Folliculitis
- Gastroparesis
- Granuloma Annulare
- Health & Fitness
- Herbal Care Products
- Hydrocele
- Ichthyosis
- Lichen Planus
- LifeStyle
- Lipoma
- Motor Neuron Disease
- Myelitis
- Osteomyelitis
- Peripheral Neuropathy
- Polycystic Kidney Disease
- Porphyria
- Premature Ejaculation
- Prickly Heat
- Rectal Prolapse
- Retinal Vein Occlusion
- Retinitis Pigmentosa
- Scleroderma
- Sebaceous Cyst
- Seborrheic Keratosis
- Supplements
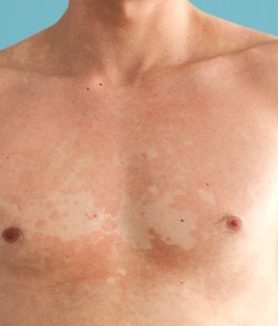
- Tinea Versicolor
- Trigeminal Neuralgia
- Uncategorized
- Uveitis
- Waldenstrom’s Macroglobulinemia
- Weight Loss